Simple solutions that boost neighborhood healthcare
by McKenzie Richards
Perhaps I should not have moved to Los Angeles given that I hate driving. Driving here – and in any city, really – can be chaotic, unpredictable and time-consuming. For a recent doctor’s appointment, I opted to walk instead. Never having walked to any healthcare appointment before, it got me thinking: What policy solutions can encourage healthcare services to be more neighborhood-oriented?
Compared to rural areas where there are not enough doctors to go around, the average city resident generally has relatively wide-ranging access to healthcare. However, even people in urban areas can struggle to get access to healthcare especially if they live in a poorer part of the city or must rely on public transportation to get to the doctor.
Localizing healthcare services in neighborhoods by increasing access, removing restrictive laws and adopting innovative new models would be a great boon to city health and create more convenient, walkable healthcare options.
Here are four simple policy solutions:
Bolstering telehealth services
Spurred by necessities wrought by the pandemic, telehealth services exploded in the last several years. Obviously, telehealth enables patients to receive the care they need from their own homes via Zoom or other online app. If more patients can meet with their doctors virtually, urban office spaces devoted to large waiting rooms and administrative staff can be used more productively.
Of course, not every health need can be treated virtually, and some people would prefer to meet with doctors in person. But, as evidenced by recent events, more people than ever are open to telehealth.
In particular, psychiatric care is well-supported by telehealth. According to research by the Centre for Urban Design and Mental Health, urban dwellers are at an almost 40-percent higher risk of depression, and 20-percent higher risk for anxiety. Psychiatrists in cities are in high demand, and telehealth opens the door for patients to receive care from anywhere. Some may feel self-conscious going in person and would prefer to meet with mental-health professionals virtually.
Meetings with nutritionists, breastfeeding consultants, follow-up care, consultations for minor medical issues, and preventative care checkups are all examples of services that can be done virtually. Even some pediatric care can be done virtually. For example, a doctor may be able to look at a picture of a strange rash or listen to the sound of a cough to make a diagnosis.
Digitally monitoring complex health problems such as interstitial lung disease (ISD) can be done safely through cutting-edge technologies. As innovation in the biotech sector continues to explode, treating and surveilling long-term diseases will become commonplace.
In urban planning, cities should tentatively prepare for the digital transformation of healthcare. The more care that can be done from home, the less individuals need to travel.

Reform scope-of-practice laws for nurse practitioners
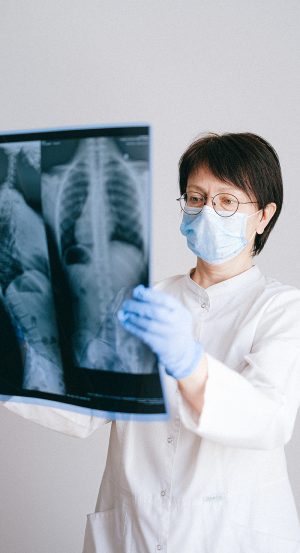
Scope-of-practice laws prohibit qualified professionals from fully practicing what they are trained to do. Nurse practitioners are highly trained medical professionals who can perform many duties similar to primary care physicians such as examinations, simple diagnoses and writing prescriptions. But these anti-competitive laws restrict these nurses from performing many healthcare services.
Scope-of-practice laws often require physician oversight of nurse practitioners. Some states only allow doctors to supervise four to five nurse practitioners. The nurse practitioners may even be required to practice within a certain distance from the supervising doctor. As a result, scope-of-practice laws severely limit the number of nurse practitioners who can work in a given area.
Unfortunately, 28 states currently require physician oversight of nurse practitioners. Loosening these laws will increase the amount of care available in urban, suburban and rural settings.
A 2017 case study of urban areas in Florida found that only 65 percent of individuals live within a five-minute drive from a primary care provider. However, that number jumped to 85 percent if nurse practitioners serving as primary care providers are included. The study highlighted the importance of nurse practitioners in meeting localized healthcare needs. Short travel times are particularly important for low-income city residents who may not have access to a car.
Wherever scope-of-practice laws exist, healthcare is artificially limited. If more nurse practitioners could practice in the city, it would allow for more offices to open throughout the city.
Get monopolistic certificate-of-need laws off the books
Certificate-of-need (CON) laws are foolhardy policies that severely limit the number of healthcare centers in cities. Essentially, CON laws give free reign to local hospitals or clinics to function as monopolies.
CON laws let existing healthcare centers decide whether a new healthcare business can open shop in a neighborhood by simply claiming the community would not benefit from additional services. That’s like Pepsi being able to prohibit the sale of Coca-Cola because “they’ve got it covered.”
Study after study finds that CON laws result in higher costs, worse health outcomes and restricted access in both urban and rural areas. Shockingly, 39 states still have CON laws on the books.
In practice, CON laws result in healthcare centers sporadically appearing, popping up in distant locations based on zoning or freeway location. Removing CON laws would correct the market, by allowing providers to go wherever there is demand.
It would also encourage decentralization of the market. Rather than hospital conglomerates running large hospital centers, removing CON law could encourage smaller healthcare centers to arise in neighborhoods. This would help meet the needs of underserved communities and provide convenient local healthcare options.


Promote the direct primary care model
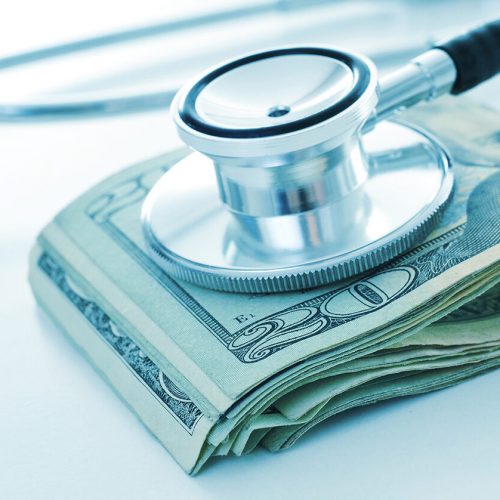
Even if a provider resides in close proximity to you, that does not necessarily mean that they take your insurance. The current insurance model may result in unnecessary travel, frustrating people who want healthcare close to home.
Direct primary care (DPC), an exciting new model, cuts out insurance altogether for routine medical treatments. Rather than pay for full health coverage through their insurance, individuals pay a low monthly fee to a local clinic that covers routine care and minor urgent care issues at no additional cost. Paired with disaster insurance, the DPC model makes a lot of sense for healthy individuals and young families.
Frequently compared to gym memberships, the DPC model truly localizes care to wherever the clinic resides and creates personal relationships between doctors and their patients.
Healthy cities begin with healthy individuals. By promoting direct primary care and telehealth and by removing harmful regulations, we can make healthcare more neighborhood-centric.
McKenzie Richards is a policy associate at the Pacific Research Institute.